GPNewsFlash October 2013
Categories: GPNewsFlash
Mesiodens Surgical Complications, The Restorative Role of Dental Hygienists in General Practice, The Birth of The CAGD and its Affiliation with The AGD, CAGD Board Meeting: CAGD Supports CDA, CAGD Dentists in the AGD Arena
Mesiodens Surgical Complications: Need for careful diagnosis, treatment planning and a safe surgical approach.
Little is reported regarding surgical complications or errors of removing mesiodens. A 7.5 years old boy presented with a palatally located mesiodens with no previous radiographs.

A Case Report by John S Bettinger, DDS, FAGD, FACD
Private practice, Santa Monica, California
The initial clinical examination revealed a visible and palpable enlargement on the hard palate slightly left of the midline and palatal to the incisal canal. The abnormal contour of the hard palate was an indication for radiographic studies.
The radiographic panoramic image revealed the presence of a mesiodens in the maxillae (Fig. 1). Periapical radiographs confirmed the location of the mesiodens to be palatal to the incisors (Fig. 2).
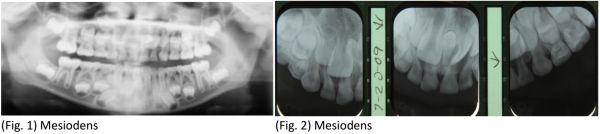
After a complete examination and consultation with the parents, it was agreed that the mesiodens would be removed. The initial surgical plan was to approach the mesiodens with an incision directly over the palatal bulge containing the mesiodens, reflecting a small flap and removing necessary bone, elevating the tooth and closing the flap. This approach would avoid the deciduous and developing central and lateral permanent incisors. The parents wanted the child sedated and I agreed that would be appropriate. Although I had an adult oral conscious sedation permit, California law requires a separate oral sedation permit for children under and including 12 years of age.
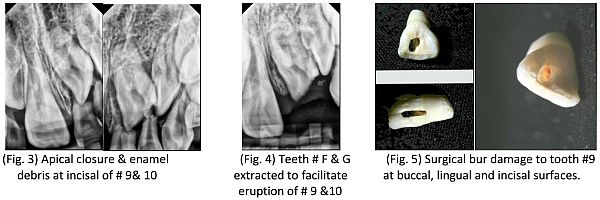
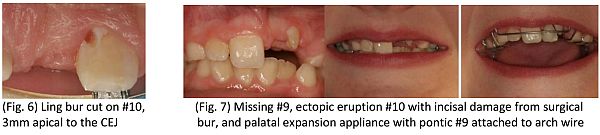
The patient’s lateral incisor (tooth #10) has recently erupted with visible extensive damage. The nick on the mesial of #10 may leave the patient with a chronic periodontal problem and a guarded long term prognosis (Fig. 6). Currently, an orthodontist is maintaining the space for the future restoration of #9 and 10 (Fig. 7).
We continually strive to learn and improve. Having always enjoyed surgery and looking back I wish that I would have had a pediatric sedation permit. We must be careful not to judge as it difficult to know what issues the surgeon faced during the actual procedure.
Editor’s Message:
The GP NewsFlash is now accepting clinical briefs for publication. Click here to check the guidelines to clinical briefs and submit your clinical brief or any question you may have to: [email protected]
The Restorative Role of Dental Hygienists in General Practice

Lee Grayson, BS, RDH Private practice, Davis, California
Few would argue that dental hygiene departments have significant growth potential for any general dental practice. Modern dental practices rely on hygienists to provide comprehensive non-surgical periodontal therapy for their patients. A hygienist who also participates in restorative evaluations significantly contributes to general dental practice growth in terms of patient satisfaction and practice profitability. Given the time constraints of today’s general dental practice, a hygienist who collects restorative data for the employer dentist is a priceless asset.
Although diagnosis is not within the scope of dental hygiene practice, skilled hygienists have been involving their patients in co-diagnosis of periodontal disease for years. Instructing patients in the significance of the data prior to the periodontal examination enables the hygienist to lead the patient to make their own diagnosis. The same technique can be employed in restorative evaluations.
Involving the patient in the examination of their oral cavity should be an interactive undertaking. An intraoral camera or simple hand mirror and a skilled guide can prepare the patient for the dentist’s examination. Whether it is the oral cancer examination, periodontal evaluation or restorative examination, the process is the same for the hygienist. Show the patient what you see and share your knowledge of its possible significance. While this is not diagnosis, it gathers data for the dentist and prepares the patient for the dentist’s diagnosis and treatment plan.
This kind of teamwork is no accident. It requires the skills and attentiveness of the hygienist. As the hygienist is completing maintenance therapy, presence of mind is important to explore not just for calculus, but also for fracture lines, root caries and recurrent decay around the margins of restorations. Documenting findings is invaluable to the dentist who has but a few minutes to complete his examination.
The dentist contributes to the success of co-diagnosis by mentoring the hygienist in the practice’s unique treatment protocols. Time invested by the dentist in developing the hygienist’s understanding of dental diagnostics and treatment planning pays huge dividends. As patients increasingly return at 3 -6 month intervals for recall visits, the hygienist needs to evaluate patient status independently. It is imperative that the hygienist assess when an unscheduled examination by the dentist is needed. With a working knowledge of the treatment plan, the hygienist can also encourage the patient to move forward with planned dentistry prior to the next scheduled examination with the dentist.
Today’s dental hygienist plays many important roles within the modern general dental practice. Being a partner in the assessment of the patient’s restorative dental needs is as important as the hygienist’s expertise in periodontal treatment. Developing the knowledge and skills needed to fulfill this role should be a priority in every general dental practice.
Lee Grayson is in private practice in Davis, California. She has been a clinical dental hygienist in both general and periodontal practices for over 40 years. She was a clinical dental hygiene instructor at the University of Texas Health Science Center in San Antonio, Texas. Lee has instructed continuing education courses in advanced periodontal instrumentation, ergonomics and sleep apnea in California and Texas.
The Birth of The California AGD and its Affiliation with The AGD

William N Langstaff, DMD, FAGD, FACD, DICOI Private practice, Villa Park, California CAGD Past president (2010)
The seed of the CAGD was planted in the summer of 1958 when a small group of dentists started meeting on a regular basis in a restaurant in Leimert Park in the Crenshaw area of Los Angeles. The name of this group was “Leimert Park Study Club”. Among the first members were Dr. Virgil Brown and Dr. Smokey Martin.
After meeting informally for about a year, the group decided to become a bit more formal and meet in a more central location, The Park Wilshire Hotel. In October of 1959 the group decided to organize as the “California Academy of General Dentistry”. Other dentists were invited to join this group too. Meetings were held quarterly and Dr. Smokey Martin was elected the first president.
Typical meetings would be for half a day, usually in the afternoon, with a dinner break, then into the evening. A Guest speaker was assigned one quarter ahead from the group. His honorarium was that he didn’t pay for dinner that meeting.
There were no annual dues and the bank account at that time was $50.00. The purpose of the group was to promote continuing education only and was totally apolitical. Certainly with the quality of this group, politics could have very well been discussed, but the understanding was that the subject was to be purely academic. The group had about 50 members and the roster looked like the who’s-who of West Coast dentists.
During Dr. Virgil Brown’s presidency (1956-1957), a group from Chicago known as the “Academy of General Dentistry” came to California to meet the leaders of the CAGD and proposed that the two groups affiliate. This group was more organized than the CAGD. Membership requirements were 50 hours of CE. The AGD also had a “Fellowship” program similar to the current program but much more informal. It took 2 years of debate – pros and cons – whether to join this Chicago group or not. At that time, the membership was about 100 in Southern California. In 1961 the CAGD decided to affiliate with the AGD and become a chapter of the AGD.
To Be Continued
The California AGD Board Meeting: Resolved, “The California AGD Supports the California Dental Association”

Chethan Chetty, DDS
CAGD Secretary
The board of directors of the California AGD recently met at the Palace Hotel in San Francisco during CDA Scientific Session on August 17th, 2013. The meeting was led by President Guy Acheson. There were several important topics discussed concerning the organization as well issues and challenges facing California dentists. Here are some of these topics:
Membership: The CAGD currently has 2346 members. California is in the top 3 regions in terms of membership along with Texas and New York.
Continuing Education: The final preparations for our Fall Meeting were announced by our meeting chair and PresidentElect, Dr. Tim Verceles. The Fall Meeting is scheduled for November 23, 2013 at the Disneyland Hotel. Dr. Steven Buchanan will lecture on endodontics. Drs. Ringrose and Costigan recently organized a very successful Mastertrack cruise to Alaska. 12-14 people attended. Everyone had a great time, with some wonderful lectures given by Dr. Lew and Dr. Lockwood, and others.

Guest: Dr Lindsey Robinson, President of CDA. Dr Robinson updated us on some issues that dentists are facing today such as MICRA (Medical Injury Compensation Reform Act) legislation and issues with Delta Dental. The CAGD board passed the following resolution: “The CAGD supports the CDA activities regarding the significant issues involving Delta Dental of California.”
CAGD Dentists in the AGD Arena (from AGD.org)
CAGD dentists Dr. Andy Alas and Dr. Diana Nguyen regularly contribute to the Daily Grind – the blog of the AGD.
In his post “Greatest Dentist Ever?”, Dr. Alas describes how his face made it to Mount Rushmore.
Dr. Nguyen, in her post “My Biologic Width, My Self”, shares her ongoing journey of getting in shape after “pan-Asian takeout while attempting to memorize information” when she was at dental school.

Dr. Andy Alas

Diana Nguyen
